|
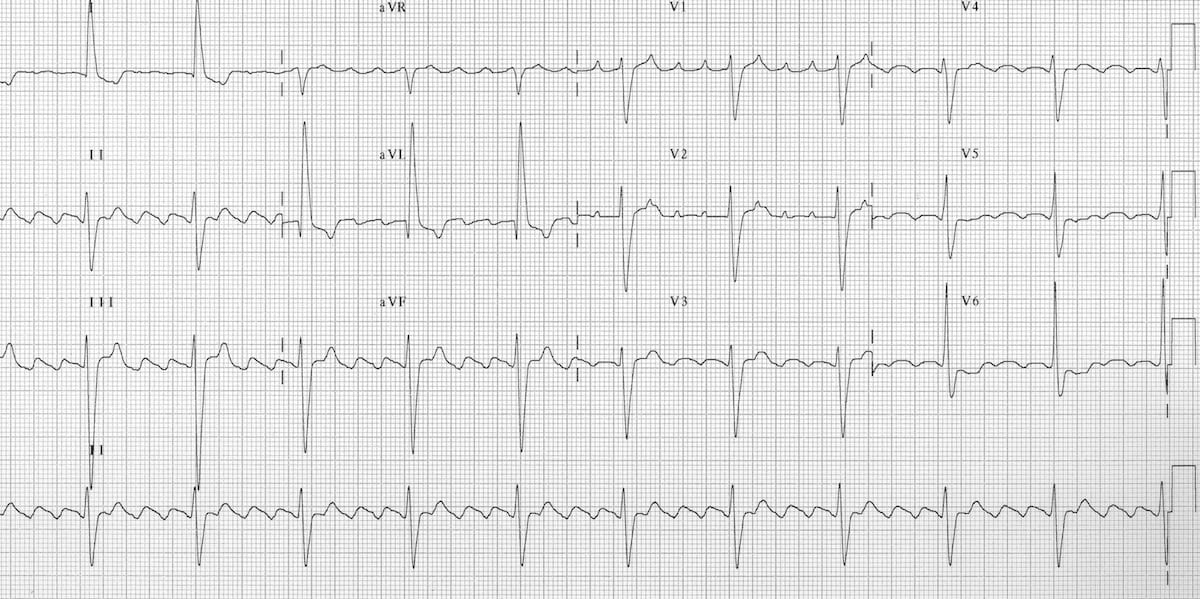
8/8/2023 0 Comments Typical atrial flutter and ecgIn some cases, however, the P-wave will be visible, either before or after the QRS complex. The P-wave is not visible in most cases, because it is hidden within the QRS complex (the atria and the ventricles are activated simultaneously, but ventricular potentials dominate the ECG). The ventricular rhythm is regular (as is the atrial) with a rate ranging between 150 and 250 beats per minute. Hence, the ventricles will be activated normally via the His-Purkinje system and therefore the QRS complexes are normal (QRS duration < 0.12 s), unless there is a intraventricular conduction defect. As it circulates within the node, it emits impulses both upwards to the atria and downwards (via His bundle) to the ventricles. 
The impulse may subsequently circulate within the atrioventricular node, as long as it encounters excitable tissue. If the refractory pathway has repolarized before the impulse has left the atrioventricular node, it may circulate back (upwards) through the previously refractory pathway, as shown in Figure 1. The impulse will only be conducted through the excitable pathway whereas it will be blocked in the refractory pathway. 
This is illustrated in Figure 1 (study this figure carefully). If an atrial impulse reaches the atrioventricular node when there are two pathways, one being refractory and the other capable of conducting the impulse, re-entry may arise. In most cases the re-entry is induced by a premature atrial beat reaching the atrioventricular node while some fibers are still refractory. AVNRT is caused by reentry in the atrioventricular (AV) nodeĪtrioventricular nodal reentrant tachycardia (AVNRT) is caused by a re-entry within the atrioventricular node. Some textbooks use the term “node” instead of “nodal”. AVNRT should not be confused with AVRT, which is the result of pre-excitation (accessory pathway).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
